Access challenges are the result of regulatory barriers that limit how healthcare can be delivered
Rule revisions
Across the country, states have modernized healthcare delivery by allowing Advanced Practice Registered Nurses (APRNs) to practice to the full extent of their education and training. North Carolina has not.
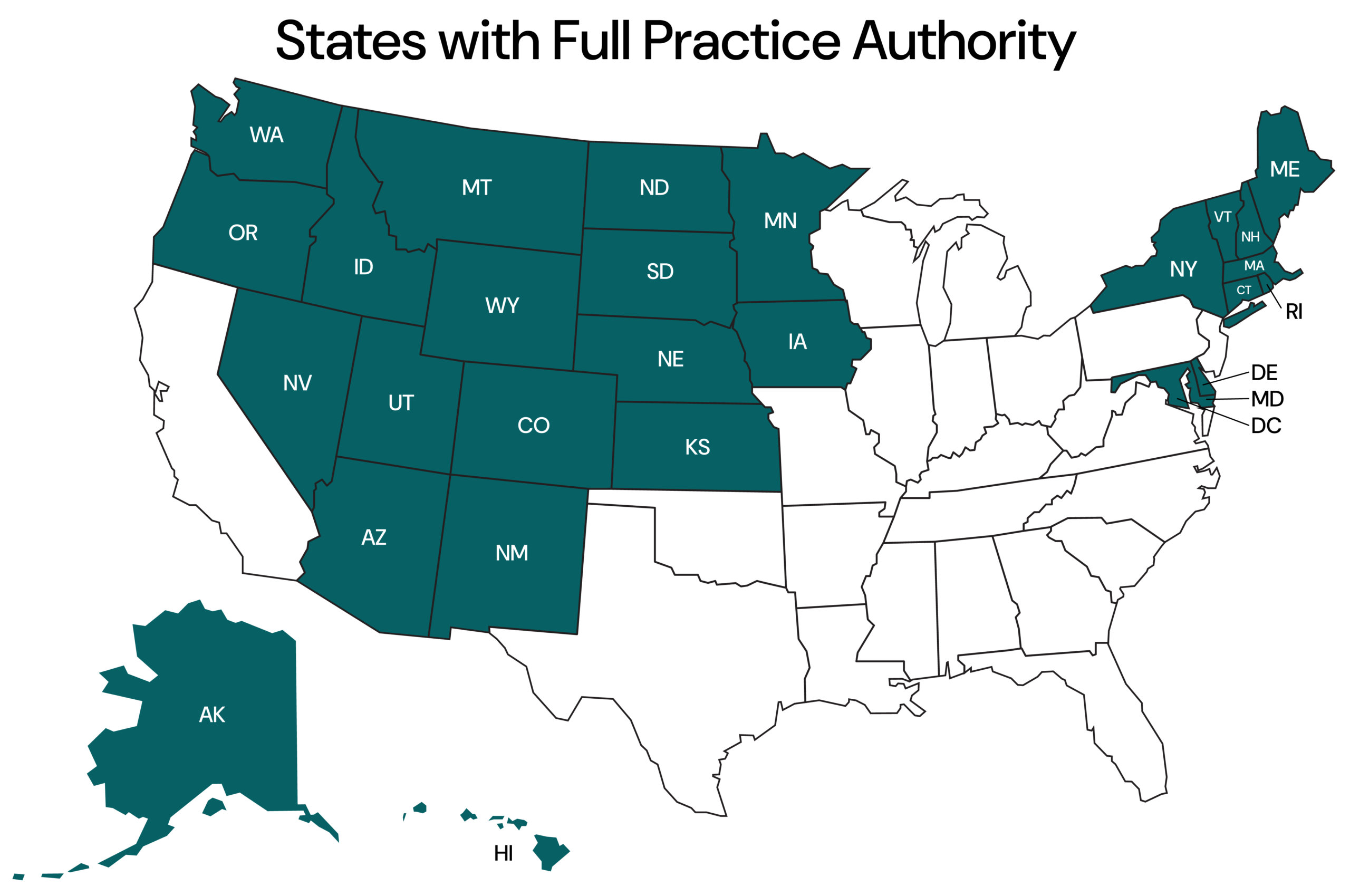
Currently, 27 states and Washington, D.C. allow full APRN practice authority. None have reversed course. These states have expanded access, maintained quality, and strengthened their healthcare systems. North Carolina remains an outlier—not because the evidence is unclear, but because outdated rules continue to restrict care.
Outdated supervision requirements
Under current law, APRNs are required to maintain a contractual collaboration agreement with a physician even when those arrangements do not reflect how care is actually delivered. These requirements add cost, create administrative friction, and limit where and how APRNs can serve patients.
Independent analysts and policy observers have noted that these supervision rules are largely superfluous—adding expense without improving quality or safety. In practice, they reduce appointment availability, discourage rural practice, and restrict patient choice.
Telehealth barriers
The same regulatory constraints that limit in-person care also restrict telehealth. Even as technology makes remote care more accessible, North Carolina’s supervision requirements prevent APRNs from fully delivering services they are licensed to provide—whether remotely or in person.
These limitations undermine one of the most effective tools for expanding access in rural and underserved areas, where telehealth can reduce travel burdens and speed up care.
Anticompetitive effects
Restrictive supervision requirements do more than limit access—they reduce competition. By preventing qualified providers from practicing independently, current rules constrain the healthcare market, limit consumer choice, and contribute to higher costs.
Free-market and business-focused organizations have increasingly raised concerns that these regulations protect legacy structures rather than patients. When competition is limited, patients pay more and wait longer.
Why these barriers persist
These restrictions persist not because they are evidence-based, but because regulatory systems are slow to change. Healthcare delivery has evolved rapidly, while oversight frameworks have not kept pace.
In contrast, states that have modernized APRN practice have done so incrementally and responsibly—updating rules to reflect how care is delivered today, not decades ago.
What modernization would change
Modernizing APRN regulations would remove unnecessary barriers while preserving patient safety and accountability.
It would:
- Expand access to primary and preventive care
- Improve telehealth availability
- Increase competition and consumer choice
- Reduce administrative costs
- Align North Carolina with national best practices
A policy choice, not a risk
At its core, what’s holding access back is not uncertainty—it is policy inertia. North Carolina has ample evidence, national comparisons, and real-world experience to act.
Modernizing APRN practice authority is not a leap of faith. It is a policy choice informed by what has already worked elsewhere and what North Carolina has already tested successfully.