Expanded healthcare coverage does not create doctors, clinics or appointment availability
Access reality
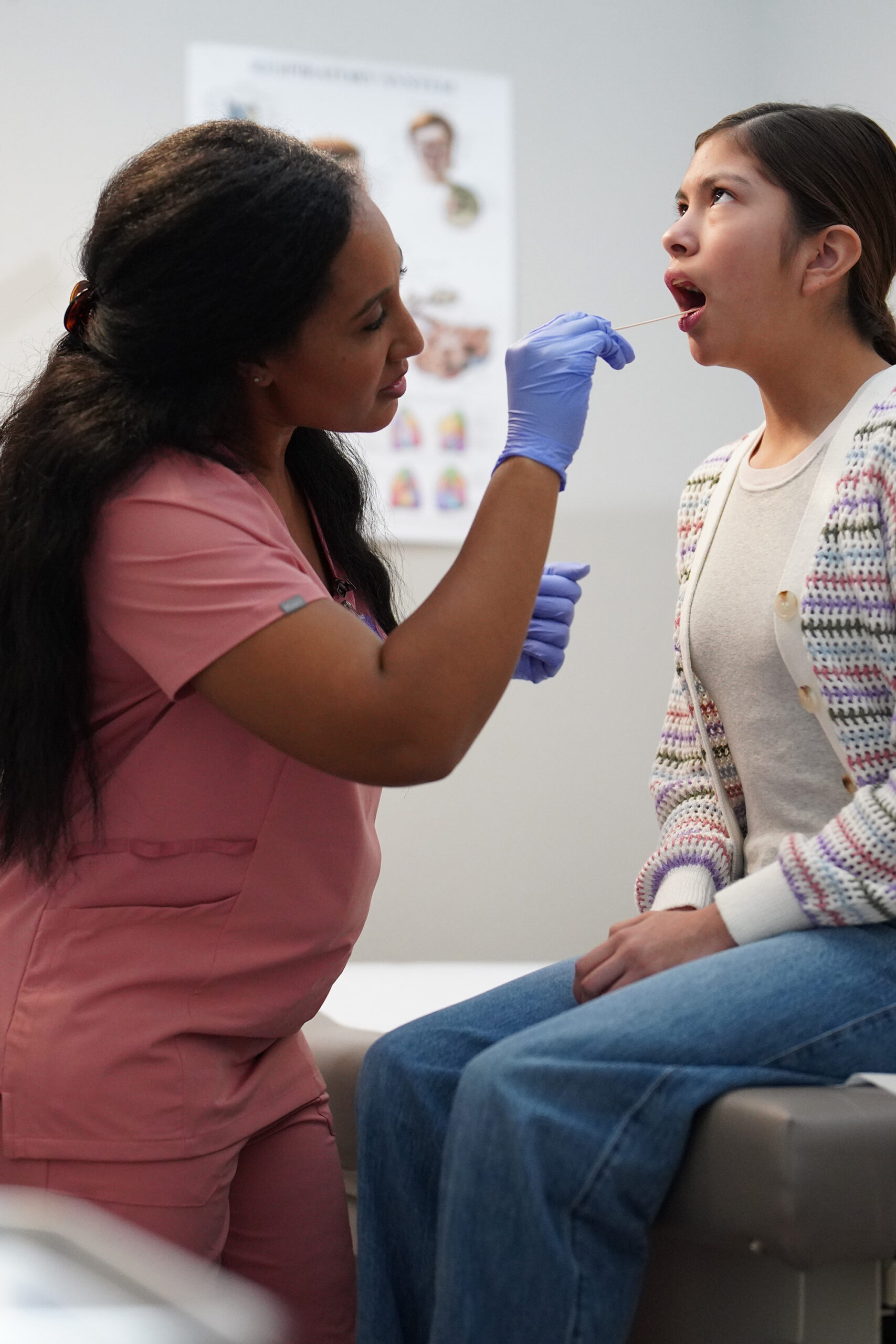
Almost 700,000 North Carolinians have gained health insurance through Medicaid expansion—a positive and important step. But across much of the state, especially in rural and underserved communities, the healthcare system did not add provider capacity fast enough to meet this surge in demand.
The result is a growing mismatch between the number of people seeking care and the number of providers available to deliver it.
In many communities, patients face longer wait times, fewer appointment options and increased travel distances for routine care. Emergency departments are often used for non-emergency needs simply because primary care access is limited.
Why this gap exists
This access gap is not the result of a single policy failure or workforce decision. It reflects a structural issue:
- Coverage policy expanded demand for care
- Workforce policy did not expand who is allowed to deliver care
Physician shortages—driven by retirements, burnout, training bottlenecks, and consolidation—have intensified nationwide. In North Carolina, these shortages are most acute in rural counties, where recruiting new physicians can take years, if it is possible at all.
Why coverage alone isn’t enough
Insurance coverage only improves health outcomes when patients can actually access care. Without sufficient provider capacity, expanded coverage can unintentionally lead to:
- Longer wait times for appointments
- Delayed diagnosis and treatment
- Higher downstream healthcare costs
- Increased pressure on hospitals and emergency rooms
Expanding coverage without modernizing care delivery limits the full benefit of Medicaid expansion and places additional strain on an already stretched system.
A capacity solution already exists
Advanced Practice Registered Nurses (APRNs) already provide high-quality primary and preventive care across North Carolina. They are trained, licensed and embedded in many of the communities facing the greatest access challenges.
However, outdated regulations restrict how APRNs can practice—requiring costly and unnecessary supervision arrangements that do not improve quality but do limit availability. Modernizing these rules would immediately expand provider capacity by allowing an existing workforce to meet patient demand.
What modernization changes
Modernizing APRN practice authority does not create new providers—it allows North Carolina to fully use the providers it already has.
This approach:
- Expands access faster than training new physicians
- Improves appointment availability in rural and underserved areas
- Reduces pressure on hospitals and emergency departments
- Improves the return on investment from Medicaid expansion
- Requires no new taxpayer funding
How this connects to the bigger picture
Addressing access without capacity is not about professional turf or ideology. It is about aligning coverage policy with workforce policy so that healthcare investments translate into real, timely care for patients.
Modernizing APRN regulations is a practical, evidence-based way to close the access gap and ensure North Carolina’s healthcare system can meet the needs of the people it serves.